Legislation proposed by U.S. Senators Bill Cassidy (R-LA) and Lindsey Graham (R-SC) would reconfigure federal funding for health coverage in Tennessee and put more decisions in the hands of our governor and state legislators. Currently, the bill does not appear to have enough votes to pass the U.S. Senate. In case that changes, the summary and analysis below discuss how the bill might impact Tennessee.
Highlights of the Graham-Cassidy Proposal
Graham-Cassidy repeals elements of the Affordable Care Act (ACA), reforms others, makes major changes to Medicaid, and returns many decisions about regulating health insurance to the states. The legislation:
- Repeals the ACA mandates that individuals buy and employers provide health insurance.
- Creates a federally-run reinsurance program to help stabilize healthcare.gov Marketplace premiums in 2018 and 2019.
- Repeals the ACA’s Medicaid expansion in 2020 for expansion states and in 2017 for non-expansion states.
- Repeals healthcare.gov Marketplace subsidies in 2020.
- Converts the money spent on Marketplace subsidies and Medicaid expansion into block grants for each state from 2020-2026.
- Slows the growth of federal spending on Medicaid by implementing per capita caps.
The bill does not provide short-term funding for cost-sharing subsidies for insurance providers.
The bill gives states broad discretion to regulate health insurance, making it difficult to predict the effect on insurance coverage and costs. States could potentially waive a variety of federal rules, such as the ACA’s essential health benefits, and instead set their own rules.
Federal Funding to Tennessee
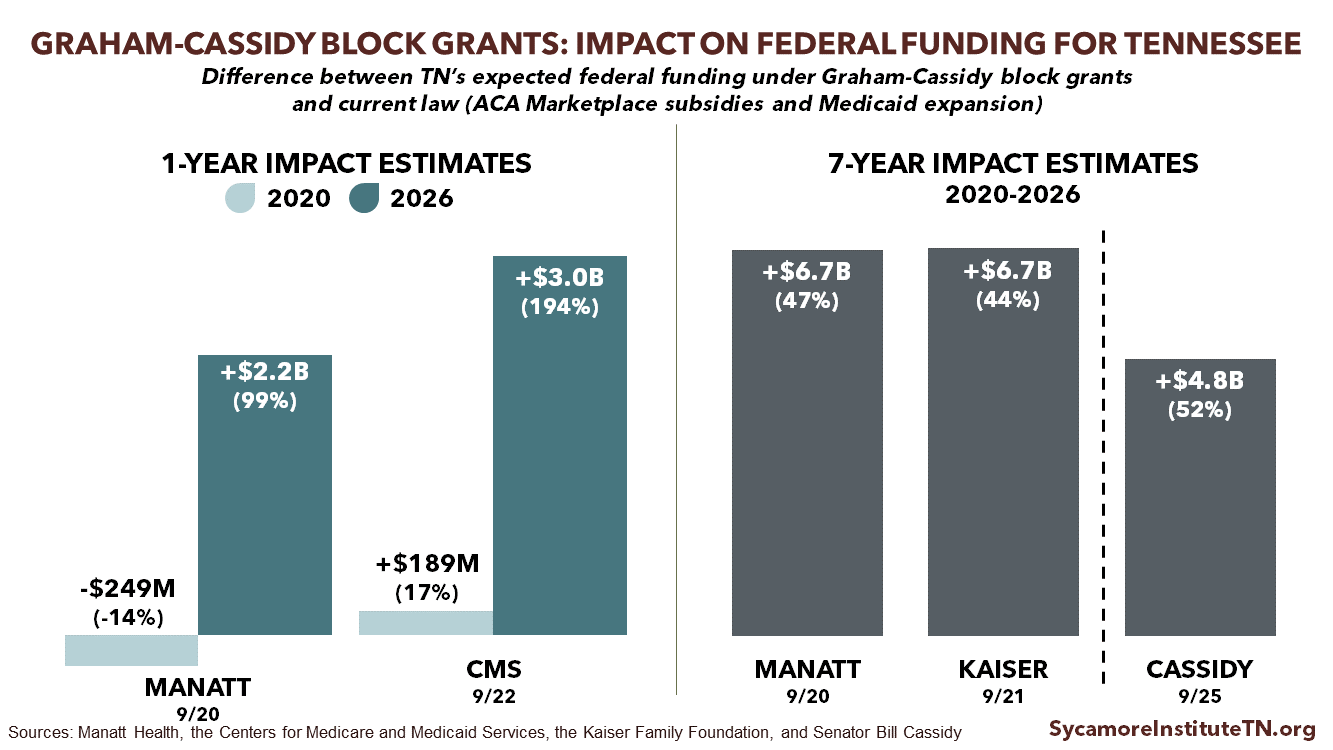
Numerous sources agree that the Graham-Cassidy block grants would increase federal funding to Tennessee in 2020-2026. The latest version of the bill produces smaller increases for Tennessee than previous versions. As the annual impact estimates show, Tennessee’s federal funding increases would grow larger as the block grant’s formula phases in.
Sources: Manatt Health (1) , Kaiser Family Foundation (2), Centers for Medicare & Medicaid Services (3), Senator Cassidy (4)
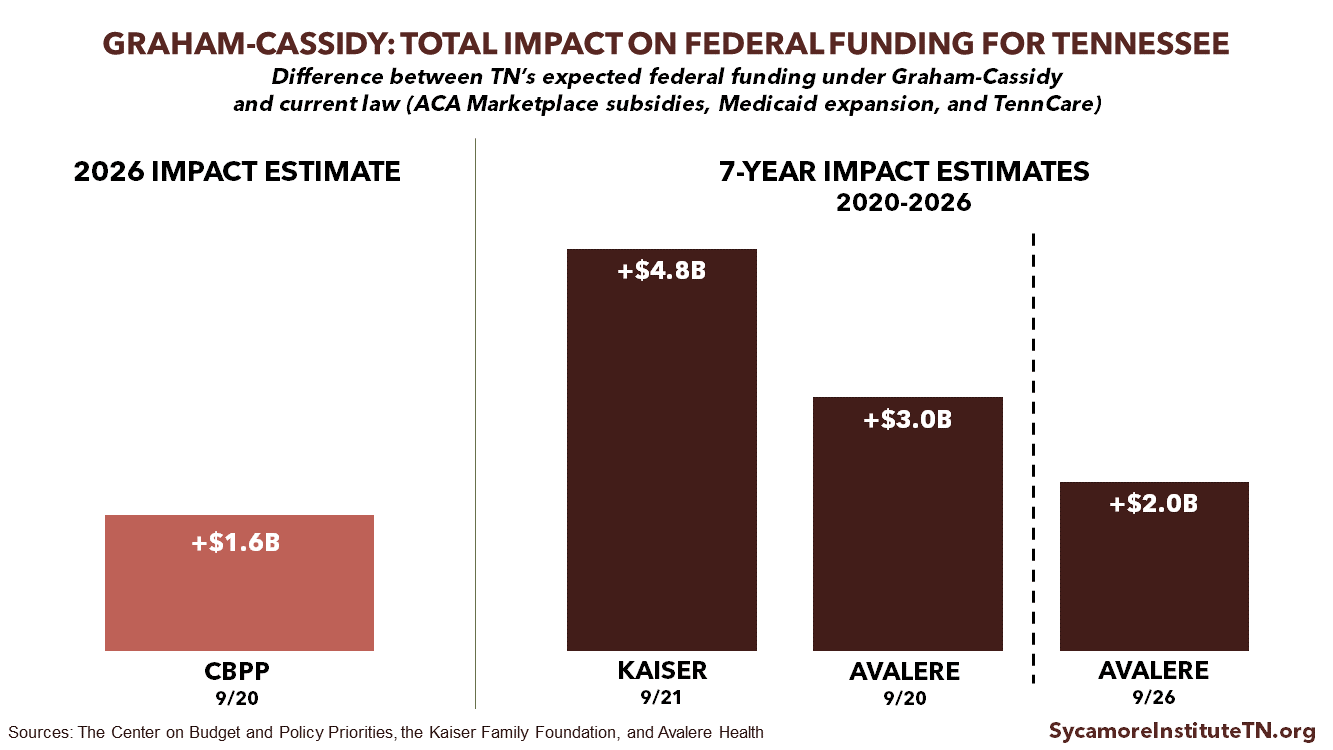
Some sources anticipate federal funding reductions for Tennessee from the Medicaid per capita cap — offsetting some of the increases from the block grant.
Sources: Center on Budget and Policy Priorities (5), Avalere Health 9/20 (6), Avalere Health 9/26 (10), Kaiser Family Foundation (2)
Federal Medicaid funding continues after 2026, but the Graham-Cassidy block grants would end unless Congress renews them. This framework could potentially lead to robust political debates over the future of these block grants.
Graham-Cassidy’s Block Grants
The Graham-Cassidy block grants reduce overall federal spending and dramatically change how it is distributed among the states. Generally, states that have higher healthcare.gov Marketplace subsidies and/or approved the ACA’s Medicaid expansion will get less money than under current law. States that have lower subsidies and/or did not expand Medicaid will get more money. The latest draft of the bill has smaller gains and losses for many states than an earlier version — likely reflecting efforts to find 50 votes.
Tennessee would get more money under the block grant through 2026 than it will under current law. The bill sponsors project our state would receive about $14B in block grant funding from 2020-2026. (4) Estimates of previous versions of the bill were about $20B over that period. (2) (1) In 2027 and beyond, this funding would fall to zero unless Congress renews the block grant. This so-called “funding cliff” provides an opportunity for future lawmakers to reevaluate the approach, which could restart a politically divisive debate.
As long as the block grant is used for health coverage, states would have broad discretion on how to spend it. For example, Tennessee could use the money to subsidize health insurance for high-cost individuals, create a state-run reinsurance program, reduce health insurance premiums and out-of-pocket costs, and/or fund private coverage for Medicaid-eligible individuals.
Tennessee would have to decide how to use its block grant no later than 3 months into the next governor’s term. States must submit their plans to the U.S. Department of Health and Human Services by March 31, 2019.
Graham-Cassidy’s Medicaid Per Capita Caps
The Medicaid financing reforms in Graham-Cassidy are similar to those in the Better Care Reconciliation Act that the Senate narrowly defeated in July. Beginning in 2020, Medicaid per capita caps for various enrollee populations would grow at the following rates:
- Elderly or Disabled Enrollees: Grows with medical inflation (CPI-M) +1% through 2024 and then with CPI-M.
- Children and Other Adult Enrollees: Grows with CPI-M through 2023 and then with general inflation (CPI-U).
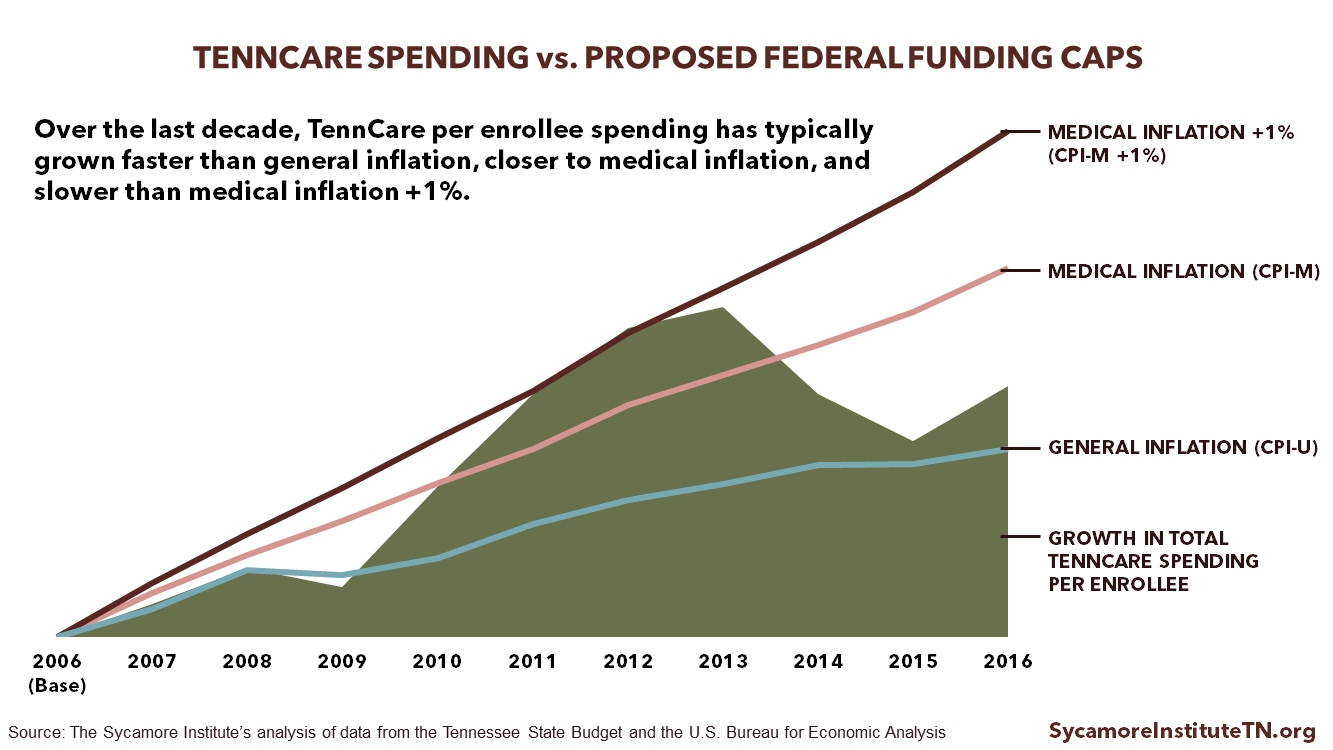
The chart below shows how these inflation measures compare to the growth of total TennCare spending per enrollee over the last decade. We defined medical inflation and general inflation here. The Kaiser Family Foundation projects Tennessee would get about $2B less in federal funding for TennCare than expected under current law.
States could qualify for bonus payments by staying below the caps and meeting certain quality requirements. These payments could not exceed $8 billion total across all states for fiscal years 2023-2026.*
Graham-Cassidy does not include any broad Medicaid design flexibilities, which would likely have to pass Congress separately due to the U.S. Senate’s budget reconciliation rules. The bill does, however, give states the option to implement a Medicaid work requirement for non-disabled, non-elderly, non-pregnant individuals.
States have the option to get all of their federal Medicaid funding for non-elderly, non-disabled adults as a block grant, which would grow with CPI-U.*
Decisions for Tennessee Policymakers
Graham-Cassidy puts many decisions about the individual health insurance market back in the hands of state governors and legislators. The bill keeps most ACA requirements about who and what health insurance in the individual market must cover, but states could waive many of these rules. For example, each state could decide to let (or not let) insurers charge different prices based on an individual’s health status, age, or several other factors (other than sex). States could also change essential health benefit requirements.
All of these decisions involve trade-offs. Waiving ACA rules could result in young and healthy Tennesseans having more access to plans with lower premiums, higher deductibles, and less comprehensive benefits — similar to the individual market pre-ACA. At the same time, older and sicker Tennesseans would likely pay more for plans with more comprehensive benefits. States’ block grant plans due in March 2019 must describe how they will “maintain access to adequate and affordable health insurance coverage for individuals with pre-existing conditions.”
The Graham-Cassidy block grants would significantly increase the federal dollars managed through Tennessee’s state budget. Today, the ACA’s Marketplace subsidies flow directly to health insurance companies. Under Graham-Cassidy, these funds would flow directly to state budgets. By 2026, Tennessee’s Graham-Cassidy block grant could amount to as much as $4.5B, according to some estimates. (3) (1) Based on FY 2017-2018 estimates, a $4.5B block grant would be the 2nd largest federal program in the state budget (behind TennCare) and a 30% increase in Tennessee’s total federal funding.
Medicaid per capita caps could increase pressure on Tennessee’s state budget. Without any broad new program design flexibility, Tennessee would have to address any gap in TennCare funding by 1) changing TennCare provider payments or eligibility, benefits, and enrollee responsibilities to the extent currently allowed under law, 2) by raising new revenues, or 3) by shifting state dollars from other budget priorities.
The Time Crunch
The nonpartisan Congressional Budget Office (CBO) expects implementation challenges “given the short time for planning and making changes.” (7) Graham-Cassidy provides states with 18 months to determine what changes they will make to the individual market — less than half the time (42 months) that was available to implement the ACA in 2010. The bill gives states until March 31, 2019 to submit plans for reforms and funding distribution. Coverage under these plans would begin on January 1, 2020.
It is unclear to what extent states will be able to rely on federal infrastructure already in place in order to meet the block grant deadlines. Graham-Cassidy would allow states to use their block grant dollars to continue the current system. However, it is unclear if or how federal infrastructure like the healthcare.gov Marketplace could be tailored to meet the needs of each state’s program. This could present an additional challenge to meeting the Graham-Cassidy timelines.
State policymakers may want to identify any needed resources to tackle Tennessee’s reforms early. A recent Milbank study found that nearly all states lacked at least some of the internal expertise, resources, or infrastructure needed to address state-level decisions required by the ACA. (8) Graham-Cassidy will require a similar (if not greater) level of state capacity for planning, vetting, and implementing health policies. To meet the deadlines, Tennessee may want to identify and plan for these capacity needs early.
Additional summaries and the full text of the Graham-Cassidy bill can be found here.
Related Work by The Sycamore Institute
How Changes to Essential Health Benefits Could Affect Tennessee
(July 13, 2017) Explains EHB and what proposed changes mean for health insurance options, premiums, benefits, and risk pools in our state.
The American Health Care Act: Rural Health and Tennesseans with Disabilities
(June 22, 2017) An analysis of the trade-offs of the AHCA for Tennessee’s 1.5 million rural residents and the 150,000 with disabilities on TennCare.
Comparing TennCare Spending Growth to the Caps Proposed by Congress
(June 23, 2017) Compares TennCare per-enrollee spending growth over the last three decades to different growth rates for Medicaid per capita cap proposals.
Medicaid Reform 101: More Than Just Block Grants
(January 26, 2017) Explain the major concepts and key terms, summarize specific federal and state reform proposals, and describe many of the difficult decisions and trade-offs our leaders are facing.
*This post was updated on Sept. 25, 2017 to reflect Avalere Health’s latest estimates and on Oct. 5, 2017 to clarify provisions related to Medicaid quality bonus payments and the Medicaid block grant option.
References
Click to Open/Close
- Boozang, Patricia, Grady, April and Guyer, Jocelyn. Update: State Policy and Budget Impacts of New Graham-Cassidy Repeal and Replace Proposal. Manatt Health. [Online] September 20, 2017. https://www.manatt.com/Insights/White-Papers/2017/Impacts-of-New-Graham-Cassidy-Repeal-and-Replace-P
- Garfield, Rachel, et al. State-by-State Estimates of Changes in Federal Spending on Health Care Under the Graham-Cassidy Bill. Kaiser Family Foundation. [Online] September 21, 2017. http://www.kff.org/health-reform/issue-brief/state-by-state-estimates-of-changes-in-federal-spending-on-health-care-under-the-graham-cassidy-bill/.
- Centers for Medicare and Medicaid Services (CMS). Estimated State Funidng Amounts under Current Law compared to Graham-Cassidy. [Online] September 22, 2017. https://www.documentcloud.org/documents/4058669-CMS-Graham-Cassidy.html.
- Cassidy, Senator Bill. Illustrative State‐by‐State Impact of Graham‐Cassidy‐Heller‐Johnson (GCHJ) Market‐Based Health Care Grant Program (Section 106), CY 2020-2026. U.S. Senate. [Online] September 25, 2017. https://www.cassidy.senate.gov/imo/media/doc/GCHJ%20State-by-State%20Impact%20(002).pdf.
- Leibenluf, Jacob, et al. Like Other ACA Repeal Bills, Cassidy-Graham Plan Would Add Millions to Uninsured, Destabilize Individual Market. Center on Budget and Policy Priorities. [Online] September 20, 2017. https://www.cbpp.org/research/health/like-other-aca-repeal-bills-cassidy-graham-plan-would-add-millions-to-uninsured.
- Carpenter, Elizabeth and Sloan, Chris. Graham-Cassidy-Heller-Johnson Bill Would Reduce Federal Funding to States by $215 Billion. Avalere. [Online] September 20, 2017. http://avalere.com/expertise/managed-care/insights/graham-cassidy-heller-johnson-bill-would-reduce-federal-funding-to-sta.
- Congressional Budget Office. Preliminary Analysis of Legislation That Would Replace Subsidies for Health Care With Block Grants. [Online] September 26, 2017. https://www.cbo.gov/system/files/115th-congress-2017-2018/costestimate/53126-health.pdf.
- Forest, Pierre-Gerlier and Helms, W. David. State Policy Capacity and Leadership for Health Reform. Milbank Memorial Fund. [Online] April 10, 2017. https://www.milbank.org/publications/state-policy-capacity-leadership-health-reform/.
- Kaiser Family Foundation. States and Medicaid Provider Taxes or Fees. [Online] June 27, 2017. http://www.kff.org/medicaid/fact-sheet/states-and-medicaid-provider-taxes-or-fees/.
- Sloan, Chris and Kane, Richard. Updated Analysis: Revised Graham-Cassidy Bill Would Reduce Federal Funding to States by $205B. Avalere. [Online] September 26, 2017. http://avalere.com/expertise/managed-care/insights/graham-cassidy-heller-johnson-bill-would-reduce-federal-funding-to-sta.